NEWS

American Epilepsy Society (AES) 2023 Annual Meeting Highlights

The Davis Lab presented many posters and talks at this year’s AES Annual Meeting in Orlando!
Talks

Nishant Sinha, PhD (Talk at SIG Neuroimaging Panel): Scalable quantitative methods to map epileptic networks and guide epilepsy surgery
Posters
Ryan Gallagher, MD student: Spatial Extent of Interictal Intracranial EEG Abnormalities Relates to the Focality of Epileptic Networks
Related paper: Quantifying interictal intracranial EEG to predict focal epilepsy.
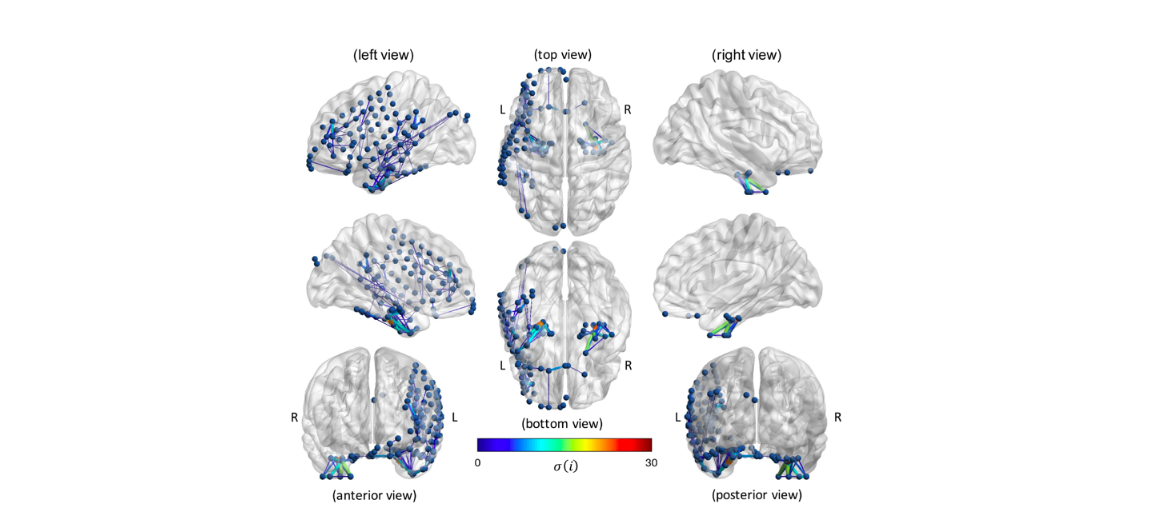
 Marc Jaskir, PhD Student: Characterizing iEEG-fMRI Coupling in Epilepsy Patients Across Seizure States and Tissue Types
Marc Jaskir, PhD Student: Characterizing iEEG-fMRI Coupling in Epilepsy Patients Across Seizure States and Tissue Types
Rationale:
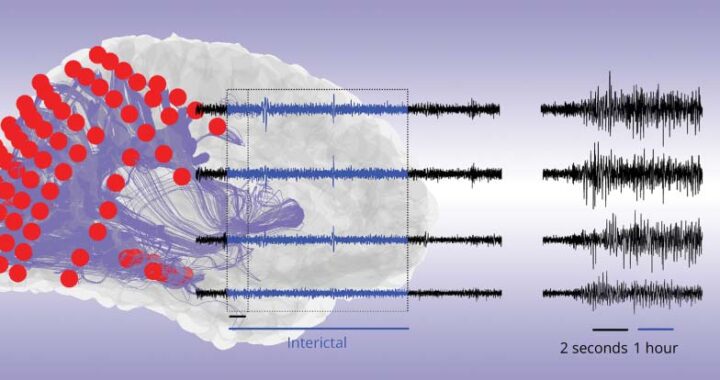
Intracranial EEG (iEEG) is an essential tool for seizure localization in epilepsy patients. However, iEEG is a highly invasive diagnostic procedure and its incomplete spatial coverage imposes limitations for whole-brain functional mapping approaches, which may reveal global network properties that are relevant to seizure onset and propagation. Multimodal approaches combining iEEG with functional magnetic resonance imaging (fMRI) may afford complementary measures of functional organization that exploit each modality’s strengths in temporal resolution and spatial coverage, respectively. However, iEEG-fMRI coupling is poorly understood1 and their relationship is further complicated by modality-specific differences between grey and white matter signal properties2,3 which are understood to change over ictogenesis. Therefore, we thoroughly characterized iEEG-fMRI coupling in epilepsy patients during different stages of ictogenesis and across different tissue types.
Methods:
Using resting state fMRI and interictal, preictal, and ictal iEEG data from 32 epilepsy patients, we evaluated differences in average iEEG-fMRI correlations and the associations between their graph theoretic properties (global efficiency) across different tissue types, seizure states, and frequency bands. We also used dynamic functional connectivity to elucidate seizure state-specific changes in iEEG-fMRI coupling over time.

Alfredo Lucas, MD/PhD Student:
Disparities and Algorithm Bias in Natural Language Processing of Epilepsy Outcomes
Exploring Cortico-cortical Evoked Potentials as a Marker of the Seizure Onset Zone
Guiding Intracranial EEG Implantation in Epilepsy Using Normative Brain Imaging
Improved Seizure Onset-Zone Lateralization in Temporal Lobe Epilepsy Using 7T Resting-State fMRI: A Direct Comparison with 3T
Multidien Cycles in Interictal Background Features of Long-Term EEG Recordings
Quantitative Intracranial EEG Abnormalities Across States of Consciousness in Drug-resistant Epilepsy
Role of Morphology in Interictal Spikes to Elucidate Seizure Generation
iEEG-recon: A Fast and Scalable Pipeline for Accurate Reconstruction of Intracranial Electrodes and Implantable Devices
Related papers:
Resting state functional connectivity demonstrates increased segregation in bilateral temporal lobe epilepsy
Dan Zhou, MD:
MEG Slow Wave Activity Associated with Brain Tumors in Patients with and Without Epilepsy
Rationale:
Epilepsy is prevalent in nearly half of patients with primary brain tumors. Recent evidence suggests that brain tumors can generate abnormal electrical activity in peritumoral tissue and affect local brain networks. Magnetoencephalography (MEG), a noninvasive imaging tool used for the functional mapping of eloquent cortex and localization of epileptogenic brain regions, has been used for cortical mapping prior to resective surgery. However, the evaluation of spontaneous interictal activity is often omitted. We aimed to characterize the interictal activity, including epileptiform discharges and slow activity, of patients who received presurgical MEG and compare the results between patients with and without brain tumor-related epilepsy (BTRE).
Methods:
We performed a retrospective analysis of the spontaneous interictal recordings in MEG during awake and sleep states in patients with primary gliomas who were recorded at the University of Nebraska Medical Center from July 2021 to March 2023. Focal slow wave activity (delta-theta band) was identified and processed for source localization using the equivalent current dipole method with Neuromag and Curry software. Dipoles were accepted when the goodness of fit was ≥80% and superimposed onto the individual patient’s brain MRI. A cluster was formed when ≥5 dipoles were localized closely together. Pre- and post-operative brain MRIs were used to determine tumor and resection sizes and locations, and the dipoles were then localized against the tumor resection sites.
Nishant Sinha, Ph.D, Publishes Cover Article in Neurology
 Nishant Sinha, PhD, a post-doctoral research fellow in the Center for Neuroengineering and Therapeutics, published a paper last month in Neurology that was featured as the cover article. The paper, titled “Intracranial EEG Structure-Function Coupling and Seizure Outcomes After Epilepsy Surgery”, examined the relationship between brain structure and function to determine the extent to which this relationship affects the success of the surgery in controlling seizures. This study showed that the strength of structure-function connectivity coupling may play a crucial role in determining the success of epilepsy surgery.
Nishant Sinha, PhD, a post-doctoral research fellow in the Center for Neuroengineering and Therapeutics, published a paper last month in Neurology that was featured as the cover article. The paper, titled “Intracranial EEG Structure-Function Coupling and Seizure Outcomes After Epilepsy Surgery”, examined the relationship between brain structure and function to determine the extent to which this relationship affects the success of the surgery in controlling seizures. This study showed that the strength of structure-function connectivity coupling may play a crucial role in determining the success of epilepsy surgery.
Click HERE to read the full article.

ICTALS Highlights 2022
Read below to learn more about the projects that were presented at this year’s ICTALS conference by members of the Davis Lab!
Quantifying Seizure Spread Using Deep Learning Algorithms to Localize Seizure Onset
Andrew Y. Revell, Erin C. Conrad, Brittany Scheid, Brian Litt, Kathryn A. Davis
- Question: How can we best quantify seizure spread captured on EEG?
- Methods: Researchers trained three deep learning algorithms on intracranial EEG data from 13 patients to classify interictal and ictal states on each channel.
- Results: The deep learning models, along with line length, were able to differentiate interictal and ictal states in five test-set patients with varying levels of robustness.
- Conclusion: Deep learning models can be used to quantify seizure spread and may localize seizure onset better than simple features when combined with predictive network models of spread.
Intracranial EEG structure-function coupling predicts surgical outcomes in focal epilepsy
Nishant Sinha, John S. Duncan, Beate Diehl, Fahmida A. Chowdhury, Jane de Tisi, Anna Miserocchi, Andrew W. McEvoy, Kathryn A. Davis, Sjoerd B. Vos, Gavin P. Winston, Yujiang Wang, Peter N. Taylor
- Hypothesis: In epilepsy, surgery alters the structural brain network to control seizure activity emerging at the functional level. Given that surgery is a structural modification aiming to alter the function, researchers hypothesized that strong structure-function coupling improves post-operatively seizure control.
- Methods: Researchers constructed structural and functional brain networks in 39 patients with medication-resistant focal epilepsy using multimodal data from intracranial EEG recordings, structural MRI (pre and post-surgery), and diffusion-weighted MRI (pre-surgery).
- Results: At a whole network level, seizure-free patients had stronger structure-function coupling than not seizure-free patients regardless of the choice of interictal segment or frequency band. Structure-function coupling measures had the highest feature importance relative to clinical attributes, and they predicted seizure outcomes with an accuracy of 85% and sensitivity of 87%.
- Conclusion: The underlying assumption that the structural changes induced by surgery would translate to the functional level to control seizures is valid when the structure-functional coupling is strong.
Sleep and Epilepsy
Erin C. Conrad, Andrew Y. Revell, James J. Gugger, Russell T. Shinohara, Brian Litt, Eric D. Marsh, Kathryn A. Davis
- Question: What is the effect of sleep and seizures on spikes, and do sleep and seizure-related changes in spikes localize the seizure onset zone?
- Methods: Researchers performed a retrospective analysis of intracranial EEG data from 96 patients with drug-resistant focal epilepsy.
- Results: The alpha-delta power ratio accurately classified wake from sleep periods (AUC = 0.90). A machine-learning classifier incorporating only spike rates and sleep/wake state accurately identified the seizure onset zone (AUC = 0.78).
- Conclusion: The change in spike rates surrounding seizures can be used to localize temporal versus extratemporal lobe epilepsy. Spikes are more frequent and better localize the seizure onset zone in sleep.
Epilepsy Surgery
John M. Bernabei, Nishant Sinha, T. Campbell Arnold, Erin Conrad, Ian Ong, Akash R. Pattnaik, Joel M. Stein, Russell T. Shinohara, Timothy H. Lucas, Dani S. Bassett, Kathryn A. Davis, Brian Litt
- Hypothesis: Researchers hypothesize that using a normative iEEG atlas to benchmark deviations from normal brain dynamics provides a data-driven method to identify surgical targets.
- Methods: Researchers constructed a normative iEEG atlas by augmenting a 106-subject normative iEEG atlas from the Montreal Neurological Institute (MNI) with 60 subjects carefully selected from the Hospital of Pennsylvania (HUP). Researchers quantitatively compared epileptic iEEG channels to normative data and mapped patient-specific abnormalities.
- Results: The results demonstrate that for seizure onset zones (SOZ) within the mesial temporal lobe, measures of connectivity abnormality provide greater distinguishing value than univariate measures of abnormal neural activity. Furthermore, patients with longer diagnoses of epilepsy have greater abnormalities in connectivity.
- Conclusion: This study establishes a data-driven method to guide epilepsy surgery by aggregating iEEG studies.
Read more about these projects HERE.
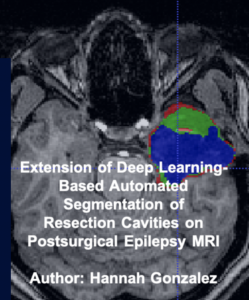
Penn Presents | Davis Lab Summer Work 2022
As a Research Assistant to Dr. Davis at Penn’s Center for Neuroengineering and Therapeutics, Hannah Gonzalez worked alongside Dr. Arnold to train a deep learning model to automate resection cavity segmentation on postoperative MRI of epilepsy patients to help physicians quantify removed brain structures.
The purpose of the project was to expand on a previous paper about Deep Learning-Based Automated Segmentation of Resection Cavities on Postsurgical Epilepsy MRI by adding a step in the data preprocessing and training of the model. After training 3 different models and running inference and the majority vote algorithm, it was determined that the Axial/Coronal model is the highest performer.
Future work in investigating the sagittal model to see how its performance can be improved.
Read more about this project HERE.
EVENTS

Dr. Davis to be ICTALS 2019 Plenary Speaker
 The International Conference for Technology and Analysis of Seizures has invited Dr. Davis to speak at its September conference ICTALS 2019 at the University of Exeter. The theme of this year’s meeting is “The Epilepsy Journey: from first seizure to treatment and beyond”. A major focus of discussion will be how recent advances in our understanding of brain dynamics can make a difference for epilepsy patients at all stages of their journey. To find out more about the event, click HERE.
The International Conference for Technology and Analysis of Seizures has invited Dr. Davis to speak at its September conference ICTALS 2019 at the University of Exeter. The theme of this year’s meeting is “The Epilepsy Journey: from first seizure to treatment and beyond”. A major focus of discussion will be how recent advances in our understanding of brain dynamics can make a difference for epilepsy patients at all stages of their journey. To find out more about the event, click HERE.

ILAE invites Dr. Davis to lecture at 33rd International Epilepsy Congress
From June 22-26, the International League Against Epilepsy (ILAE) will hold its major biennial event in Bangkok, Thailand. Dr. Davis’s lecture will be given as part of the XV Workshop on Neurobiology of Epilepsy (WONEOP). The major topic of WONOEP XV will be to discuss working definitions and classification schemes for epileptic seizures across the lifespan, improve methods of seizure recognition, detection, and classification and facilitate translation across species. To read more about the event, click HERE.

Dr. Davis to speak at Penn Medicine Neuro-Oncology Symposium 2019
On Friday, Dr. Kathryn Davis spoke at the Neuro-Oncology Brain Tumor Symposium 2019, giving a lecture entitled “Seizure Management for Brain Tumor Survivors: Current Concepts”. The symposium, designed for healthcare providers involved in the treatment of brain tumors, reviewed new treatment options in neuro-oncology. Dr. Davis’s talk was given as part of the symposium’s “Master Class in Brain Tumor Treatment & Best Practices”.

Dr. Davis to serve as a moderator at AAN Annual Meeting Neurophysiology Session
Dr. Kathryn Davis has been invited to moderate the Epilepsy and Neurophysiology sessions at the 71st Annual Meeting of the American Academy of Neurology. The meeting is to be held at the Pennsylvania Convention Center in Philadelphia from May 4-10. The Epilepsy session is to be held on Monday, May 6, and will be followed by the Neurophysiology session on Tuesday morning.
For more information about the AAN 2019 Annual Meeting, click here.

Penn Medicine Neurosurgery Grand Rounds 1.24.2019 Given by Dr. Davis
Dr. Davis will present on “Finding Epilepsy ‘Hotspots’ – Noninvasive Measures of Structure and Function,” at Neurosurgery Grand Rounds on 1.24.2019.
Location:
Smilow, TRC, 8th Floor Conference Room
Philadelphia, PA, 19104
Time: 7:00am – 9:00am